Investigations involving the uterus can feel daunting, especially when they follow symptoms such as abnormal bleeding, fertility challenges, or pregnancy loss. Many patients arrive unsure about what the test involves, how uncomfortable it might be, or what information it will provide.
This fact sheet explains what a Saline Infusion Sonography (SIS) examination is, why it is performed, and what you can expect before, during, and after the procedure. In this article, Jacqui, Lead Gynaecological Sonographer at QUFW, talks you through the SIS examination and how it helps assess the lining and shape of the uterus.
Medical disclaimer: The information in this article is general in nature and provided for educational purposes only. It does not replace medical advice, diagnosis, or treatment. Please consult your GP or specialist for personalised care.
Table of contents
- What is a saline infusion sonography (SIS)?
- Why would a SIS be recommended?
- When is a SIS performed?
- How do I prepare for my SIS appointment?
- How is the SIS procedure performed?
- What will I feel during the SIS procedure?
- How long does a SIS appointment take?
- When and how do I receive my SIS results?
- Is SIS safe?
- After the procedure: recovery and care
- Book your gynaecology scan at QUFW
- References
- Video transcript
What is a saline infusion sonography (SIS)?
A Saline Infusion Sonography (SIS) is a specialised ultrasound procedure used to assess the internal cavity of the uterus.
“An SIS is an ultrasound procedure that provides information relating to the internal cavity of the uterus,” Jacqui explains.
During the procedure, a sterile saline (salt-water) solution is gently introduced into the uterus. This fluid separates the walls of the uterine cavity, allowing the endometrial lining to be seen more clearly on ultrasound.
“An SIS uses a salty water solution inserted into the uterus, which allows visualisation of the lining of the uterus, the endometrium.”
This enhanced view helps identify abnormalities that may not be visible on a standard transvaginal ultrasound.
Why would a SIS be recommended?
You may be referred for an SIS for several reasons.
“An SIS is used to detect abnormalities of the lining of the uterus,” says Jacqui.
Common indications include:
- Abnormal uterine bleeding
- Infertility investigations
- Recurrent miscarriages
- Suspected uterine polyps or fibroids
- Congenital uterine anomalies
- Assessment of uterine shape
- Adhesions or scar tissue
SIS is particularly useful when symptoms persist but routine ultrasound findings are inconclusive.
When is a SIS performed?
Timing is important for both safety and diagnostic accuracy.
“The procedure needs to be performed between four to ten days after the first day of your last menstrual period,” Jacqui explains.
Our doctors perform the procedure after a thorough transvaginal assessment of the pelvic organs has been performed by our sonographers.
Patients are advised to contact QUFW on day one of their period to schedule the examination. If cycles are irregular or infrequent, individual advice is provided.
This timing reduces the chance of early pregnancy and allows optimal assessment of the endometrium.
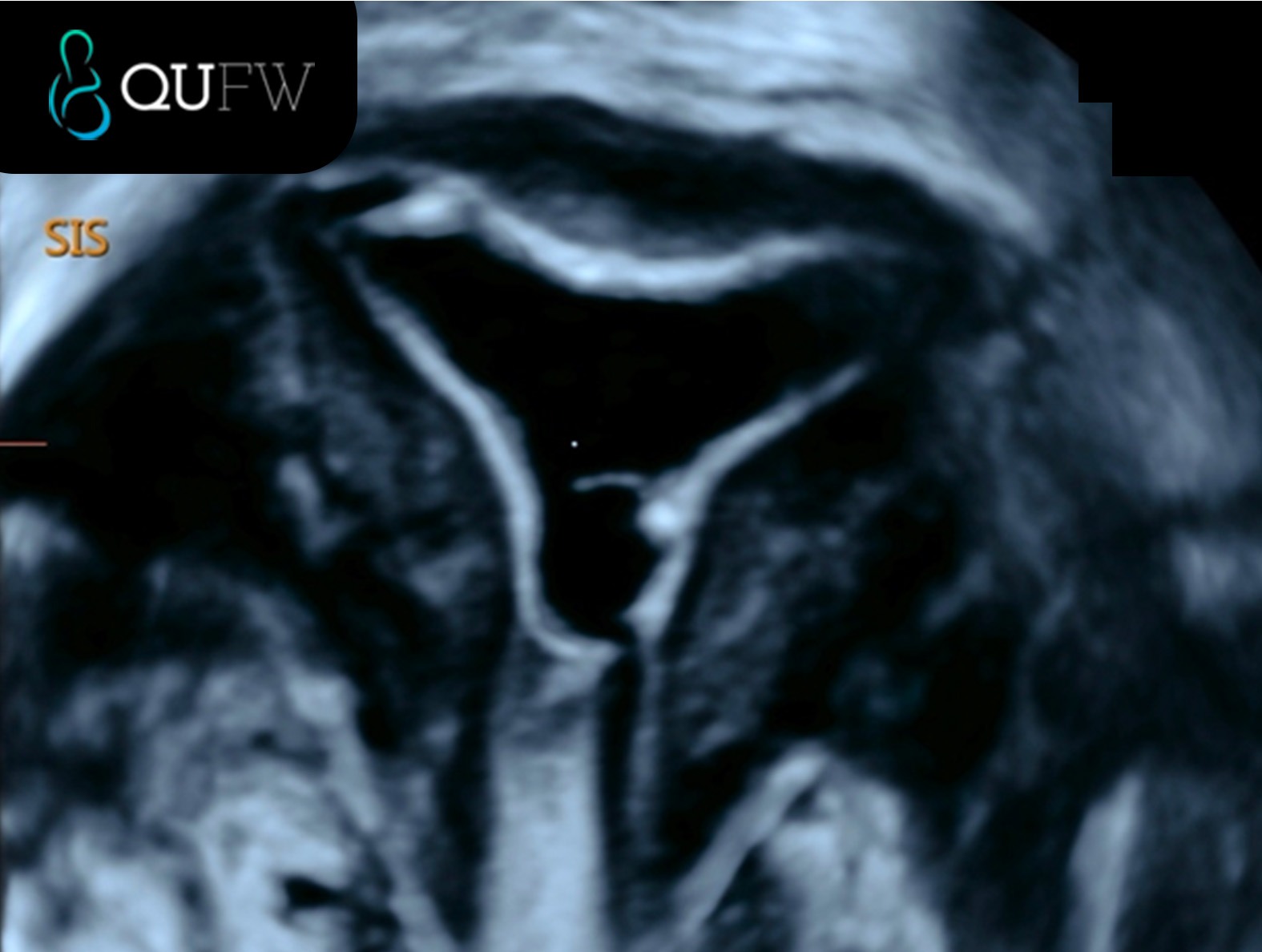
Saline Infusion Sonography (SIS) showing the endometrial cavity in the coronal plane
How do I prepare for my SIS appointment?
Preparation is simple and focused on comfort.
“You do not require a full bladder for the procedure,” Jacqui notes.
You may be asked to:
- Refrain from sexual intercourse before the procedure
- Have a pregnancy blood test if required
- Take your preferred pain medication one hour beforehand
You are welcome to bring a support person, although this is optional.
How the SIS procedure is performed
On arrival, you will complete a urine pregnancy test to confirm you are not pregnant.
A transvaginal ultrasound is performed first to assess the pelvis. Once complete, the doctor will:
- Insert a speculum
- Gently pass a thin, flexible catheter through the cervix into the uterus
“As the catheter passes through the cervix, you may feel pain,” Jacqui explains.
Once positioned, a small balloon at the end of the catheter is inflated to hold it in place. The speculum is then removed, and the transvaginal probe is reinserted.
Saline is passed through the catheter into the uterine cavity.
“This is assessed for any scarring, polyps, or fibroids that are difficult to assess on transvaginal ultrasound.”
The ultrasound captures real-time images as the cavity is distended.
What will I feel during the SIS procedure?
Sensations vary between patients.
Some may feel:
- Period-like cramping
- Pelvic pressure
- Light-headedness, warmth, or dizziness
“This should settle with time,” Jacqui reassures.
Pain relief can be used if needed, and patients are encouraged to communicate any discomfort during the procedure.
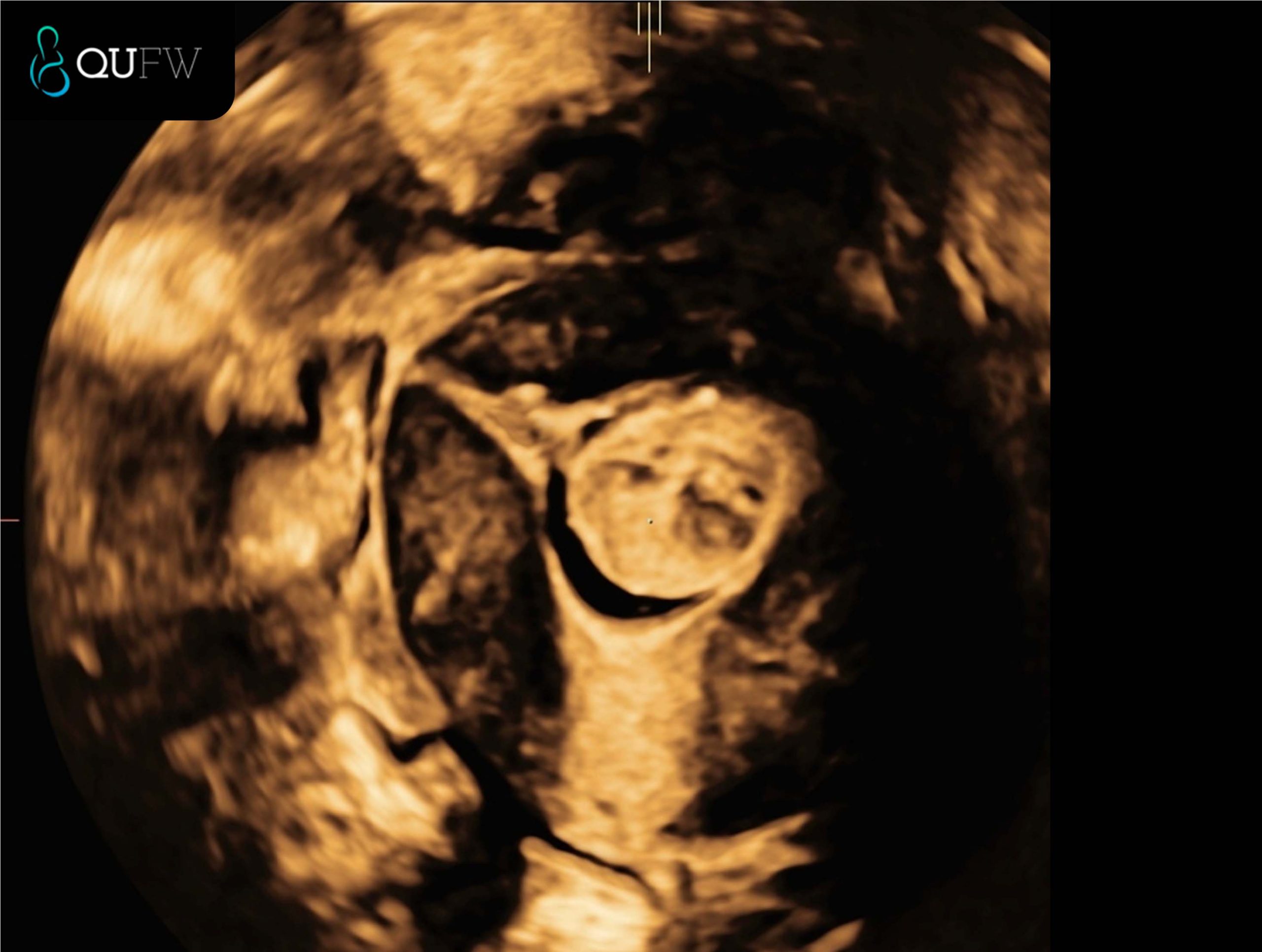
Saline Infusion Sonography (SIS) showing a 3D coronal reconstructed image of a submucosal fibroid
How long does a SIS appointment take?
“We allow 45 minutes for the procedure,” Jacqui explains.
This includes:
- The initial transvaginal ultrasound
- Preparation and setup
- The SIS itself
“The procedure itself does not take long and should be completed in about 10 minutes.”
When and how do I receive my SIS results?
Results are often discussed as the procedure is performed.
“The doctor will explain any results and any additional pathology that may be discovered.”
Your results are:
- Sent directly to your referring doctor
- Shared with you via a secure Tricefy link on your mobile
Report timing depends on the complexity of the findings and whether additional pathology is identified.
Is SIS safe?
“The SIS procedure is very safe,” says Jacqui.
SIS:
- Does not involve ionising radiation
- Does not require general anaesthetic
Pelvic infection is uncommon. You should seek medical advice if you experience:
- Severe pelvic pain
- Fever
- Green or yellow vaginal discharge
“It is also okay to have intercourse after the procedure.”
After the procedure: recovery and care
After an SIS, it is normal to experience:
- Watery or bloody discharge
- Mild bloating
- Lower abdominal discomfort or cramping
A sanitary pad is provided. Spotting or light bleeding may continue for a day or two and usually settles without treatment.
Pain relief may be used if required.
Book your gynaecology scan at QUFW
Investigations involving bleeding, fertility concerns, or pregnancy loss can feel emotionally and physically draining. Having a clear explanation of what is happening inside the uterus can provide reassurance and direction.
At QUFW, gynaecology scans are performed using evidence-based protocols in a supportive, respectful environment. Your SIS examination is designed to provide accurate information to guide diagnosis and next steps in your care.
Learn more here or contact us here.
References
- de Kroon, C. D., de Bock, G. H., Dieben, S. W., & Jansen, F. W. (2003). Saline contrast hysterosonography in abnormal uterine bleeding: a systematic review. BJOG, 110(10), 938–947. https://pubmed.ncbi.nlm.nih.gov/14550365/
Video transcript
Hi, my name’s Jacqui. I’m the lead gynaecological sonographer for QUFW and I’m going to talk you through your Saline Infusion Sonography (SIS) at QUFW. An SIS is an ultrasound procedure that provides information relating to the internal cavity of the uterus. An SIS uses a salty water solution inserted into the uterus, which allows visualisation of the lining of the uterus, the endometrium. An SIS is used to detect abnormalities of the lining of the uterus.
You may have been sent for an SIS to investigate abnormal uterine bleeding, infertility, recurrent miscarriages, or to detect uterine abnormalities such as fibroids or polyps, congenital defects, assessing the shape of your uterus, or adhesions or scar tissue. The procedure needs to be performed between four to ten days after the first day of your last menstrual period. We advise you to call the office on day one of your period to make a booking.
If you have irregular cycles or infrequent periods, please call to be advised appropriately. Some patients may be asked to refrain from sexual intercourse prior to the procedure and/or have a pregnancy blood test. You do not require a full bladder for the procedure. It is recommended to take your choice of pain medication an hour before the procedure. You may bring a support person to your appointment, but it is not a requirement.
What to expect — how is it performed?
Upon arrival at our clinic, you’ll be asked to perform a urine pregnancy test to ensure you are not pregnant. A transvaginal ultrasound is required prior to the procedure. Once the pelvic ultrasound is complete, the doctor will use a speculum and insert a thin, flexible catheter through your cervix that will go into the uterus. As the catheter passes through the cervix, you may feel pain, and once it’s in position, a small balloon on the end of the catheter will be inflated.
You may experience some additional pressure or period-like pain. This should settle with time. The speculum will then be removed and the transvaginal probe will be inserted again so we can visualise the procedure. Saline, a salt-water solution, is passed through the catheter to check the cavity of the uterus. This is assessed for any scarring, polyps, or fibroids that are difficult to assess on transvaginal ultrasound. The transvaginal probe captures real-time images of the cavity.
When the procedure is finished, the catheter and probe will be removed. Some patients may feel lightheaded, hot, or dizzy during the procedure. Some women may experience mild cramping that is similar to period pain. This will resolve shortly after the procedure, and pain relief can be used to alleviate these symptoms. If this occurs, please let either the doctor or sonographer know, and they will try to make you feel more comfortable.
We allow 45 minutes for the procedure. This includes the transvaginal ultrasound and setup. The procedure itself does not take long and should be completed in about 10 minutes.
When will I get the results of the procedure?
As the procedure is performed, the doctor will explain any results and any additional pathology that may be discovered. Your results will also be sent directly to your referring doctor. You’ll also receive a copy of the report sent to you via a link called Trisify to your mobile. The time taken for your doctor to receive the written report will depend on the complexity of the examination and whether there is any additional pathology that has been seen.
Immediately after the procedure, you may notice a watery or bloody discharge. This is the saline that was inserted through the catheter. You’ll be provided with a sanitary pad for this reason. It is normal after an SIS to experience some bloating, mild lower abdominal pain, or cramping. This may be treated with any pain medication suitable for you. Bleeding and spotting are common side effects and should settle over the next couple of days.
The SIS procedure is very safe. An SIS does not require ionising radiation or a general anaesthetic. It is not normal to experience bad pelvic pain, fever, or smelly vaginal discharge that is green or yellowish in colour. Pelvic infection is uncommon following the procedure, but if these symptoms arise, contact your GP or referring doctor as soon as possible. It is also okay to have intercourse after the procedure. If you have any concerns, please contact the referring doctor.
====================
Content Disclaimer
The information provided on this website is for educational and informational purposes only. It is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your obstetric doctor or other qualified provider with any questions you may have regarding a medical condition or treatment and before undertaking a new healthcare regimen.
The content on this website is not intended to be a comprehensive source of information on any particular topic and should not be relied upon as such. The authors and publishers of this website are not liable for any damages or injury resulting from the use or misuse of the information provided on this website.

0 Comments